What is Deep Brain Stimulation Surgery?
Deep brain stimulation (DBS) surgery is a surgical procedure used to help those struggling with movement disorders such as essential tremor. During this procedure, wires tipped with electrodes are implanted in areas of the brain that regulate motor symptoms. This wiring funnels through the neck and connects to an impulse generator (IPG) battery implanted under the collarbone. The IPG provides electrical impulses, which can be controlled by the patient via controller.
Learn more about whether deep brain stimulation, including what it’s used to treat, how it works, and its efficacy. Read our post in full or navigate to your desired section by selecting one of the links below:
Contents
What does deep brain stimulation surgery treat?
Deep brain stimulation is used to treat movement disorders including essential tremor (ET), Parkinson’s disease (PD), dystonia, and psychiatric conditions including obsessive compulsive disorder (OCD). Generally, deep brain stimulation is only used in severe cases of movement disorder, when the patient has been unable to find relief from other treatments.
Deep brain stimulation is also currently being considered as a treatment option for the following conditions:
- Alzheimer’s disease
- Addiction
- Multiple sclerosis
- Depression
- Chronic pain
- Traumatic brain injury
- Tourette syndrome
- Stroke recovery
- Thalamic pain syndrome
- Anorexia nervosa
How does deep brain stimulation improve movement disorder symptoms?
While experts don’t fully understand exactly how deep brain stimulation works, it’s believed to regulate abnormal electrical signaling patterns in the brain. Brain cells communicate with each other via electrical signals to control normal movement and other functions; with conditions like ET, these signals are irregular, which can affect motor control. DBS is thought to interrupt these irregular signaling patterns, allowing your brain cells to communicate more smoothly and reduce motor function issues.
Who is a candidate for deep brain stimulation?
In order to be considered a good candidate for deep brain stimulation (DBS), patients must undergo an extensive evaluation process. Generally, a team of specialists including a neurologist, neurosurgeon, neuropsychologist and psychiatrist must assess patients prior to this procedure.
An individual with essential tremor may qualify for DBS if they are living with:
- Debilitating symptoms of essential tremor that interfere with quality of life and are not responsive to maximal doses of medications.
Many patients living with movement disorders such as essential tremor opt for alternative, less-invasive treatments, due to the risks related to these surgical procedures.
Deep Brain Stimulation Procedure
1. Before the procedure
Before undergoing surgery, patients are put through a round of tests, including X-rays, blood tests, and electrocardiograms, and MRIs. They must consult with a multidisciplinary team of experts, which may include neurologists, brain surgeons, and movement disorder specialists.
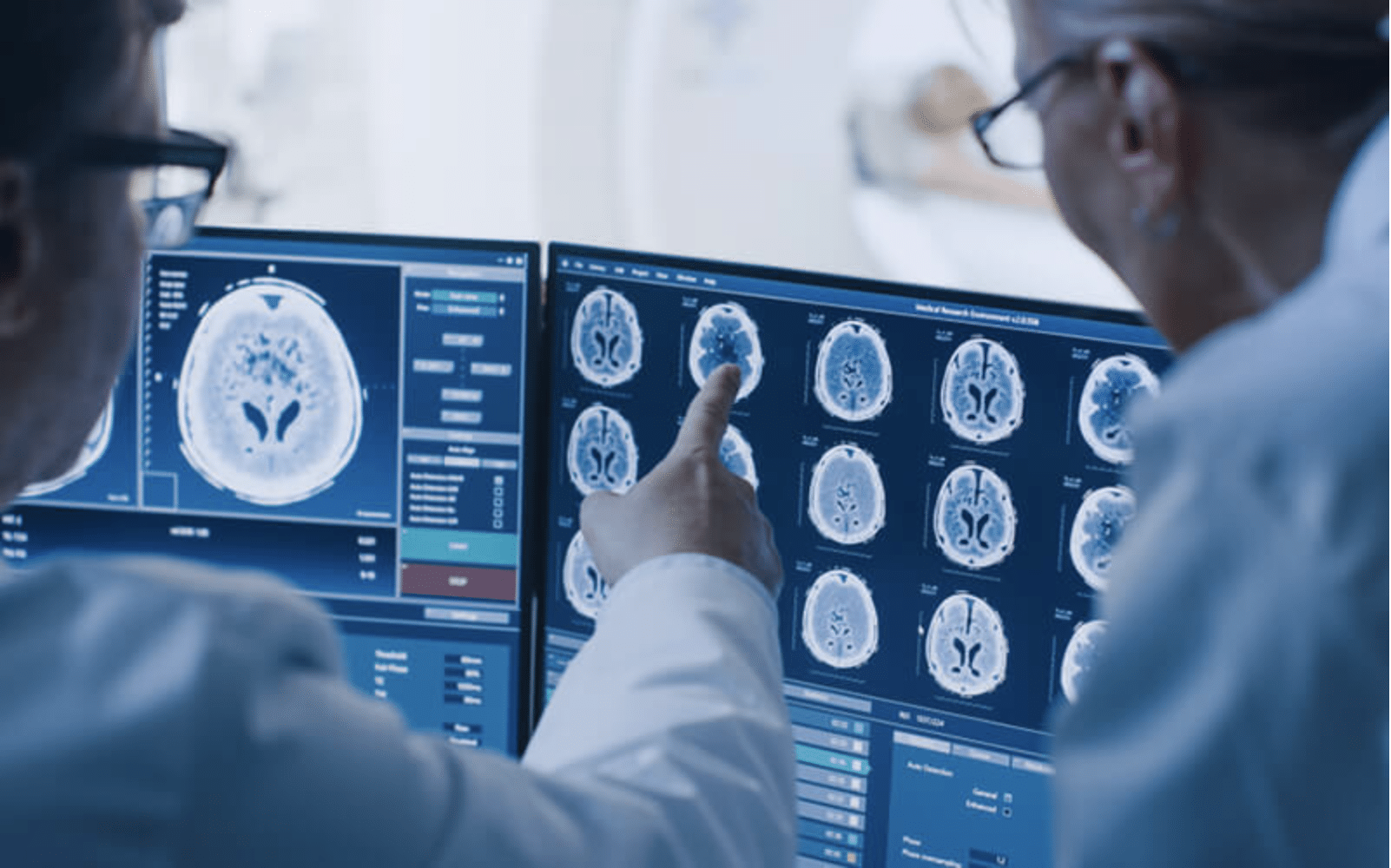
After reviewing a patient’s symptoms, medications, and memory and thinking performance, the health care team may recommend them for surgery
2. During the procedure
There are two stages of a deep brain stimulation procedure:
Brain surgery stage
During the first portion of the DBS procedure, the health care team fits the individual with a special head frame designed to stabilize the head during the procedure. Then, magnetic resonance imaging (MRI) is used to map the brain, identifying the areas where electrodes should be placed.
In some cases, the patient is kept awake and a local anesthetic is applied. This way, the patient can answer questions and perform tasks to ensure that the electrodes are properly positioned. In other cases, surgery may be done under general anesthesia; in these situations, the medical team will use brain imaging to guide the electrodes to the appropriate areas while the patient is asleep.
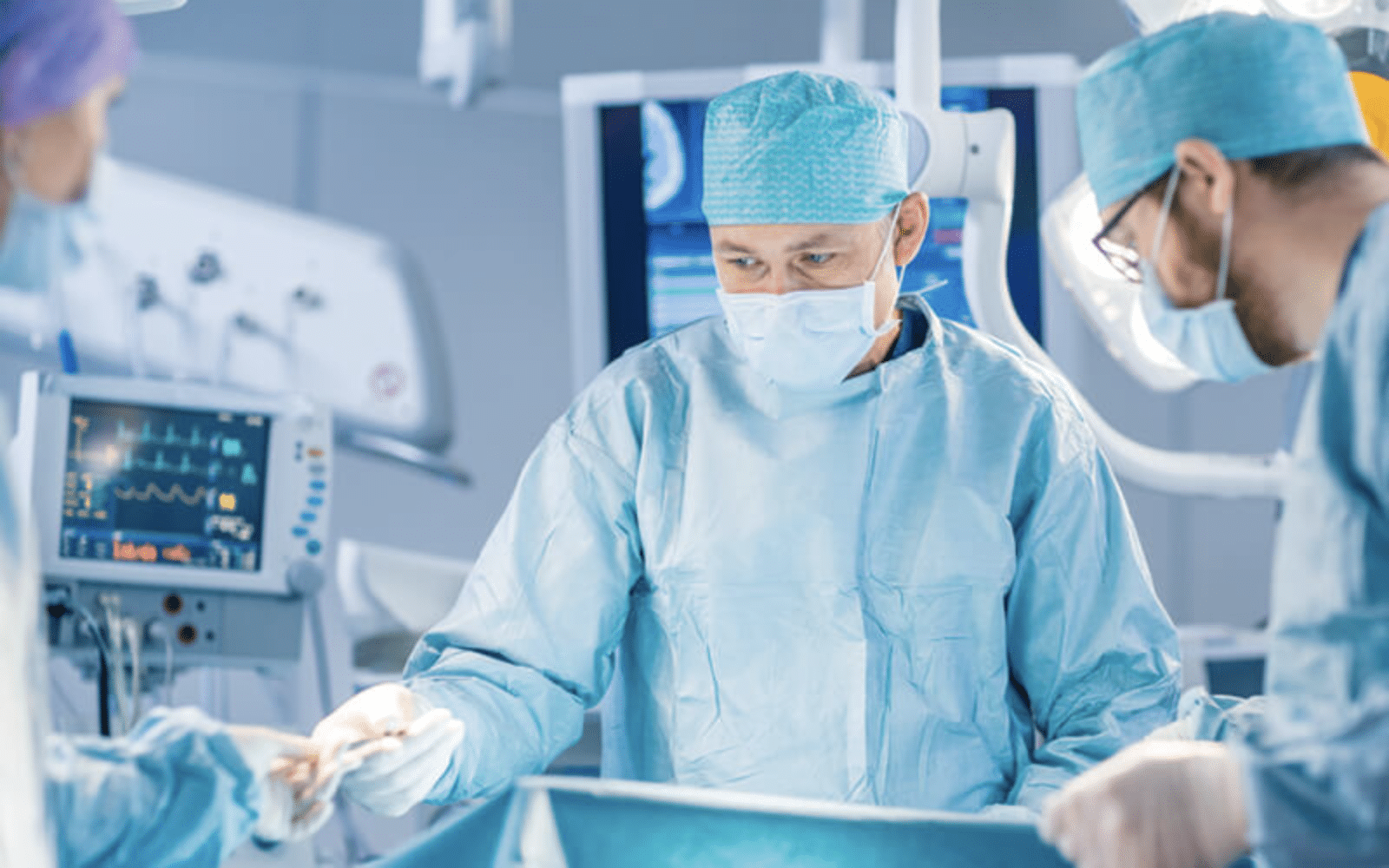
After the MRI is complete, surgery begins. The surgical team will drill two quarter-sized holes on the left and/or right side of the skull. Through these holes, they’ll insert a recording electrode, attached to a wire known as the lead. For treatment of essential tremor, these electrodes are placed in areas of the brain, typically the Ventral Intermediate Nucleus of the thalamus, associated with tremors.
Chest Surgery stage
Once the electrodes are in place, the surgeon must implant a battery-powered stimulator under the skin of the chest, near the collarbone. The long wires implanted in the head feed into this stimulator; once turned on, the stimulator sends electrical pulses to block any abnormal nerve signals that may be resulting in tremors.
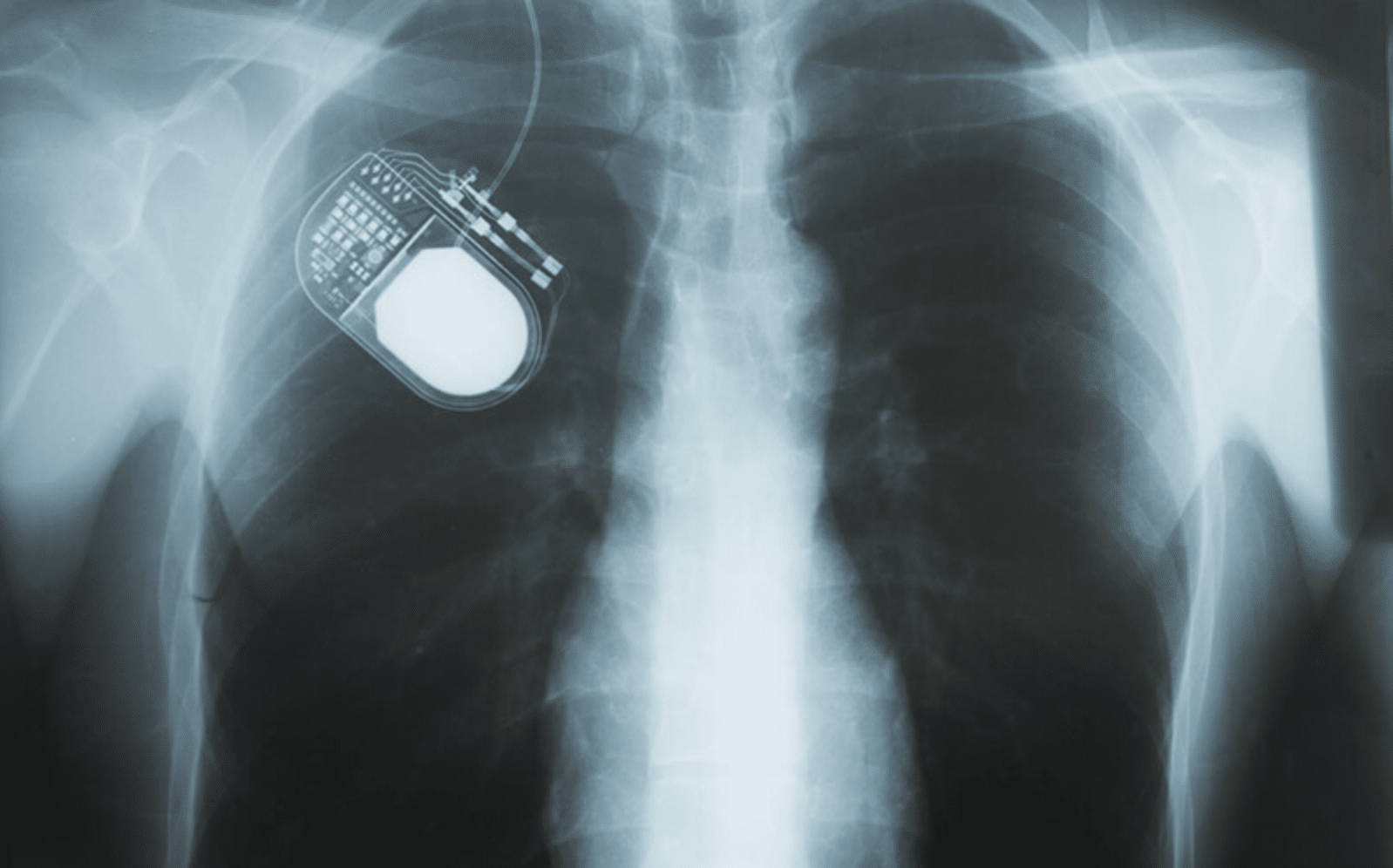
In total, a deep brain stimulation system has three main parts implanted in the body:
- Neurostimulator: Battery-powered device that generates electric pulses, and is placed under the skin near the collarbone
- Insulated wires: Carry the electrical pulses from the neurostimulator up to the scalp
- Implanted Electrodes: Deliver the electrical pulses from the wire to the areas of the brain responsible for the tremors
3. After the procedure
A few weeks following deep brain stimulation surgery, the patient will meet with their medical team to program the device, effectively “tuning” it to deliver the perfect amount of stimulation to best minimize symptoms. Following the surgical procedure, it can take anywhere between a few months and a year for doctors to adjust the device settings to best suit a patient’s unique needs.
What are the risks of deep brain stimulation surgery?
Any type of surgical procedure comes with a certain amount of risk.
Surgery complications may include:
- Bleeding within the brain
- Infection
- Stroke
- Breathing issues
- Nausea
- Heart problems
- Seizures
Deep brain stimulation for essential tremor is only used in severe cases. Generally, this type of essential tremor treatment is reserved for individuals who do not respond to other forms of treatment, including non-invasive therapies like Cala Trio, or pharmaceutical medication.
In addition to surgical risks, there are many possible side effects that a patient may experience following a deep brain stimulation procedure. These include:
- Headache
- Seizure
- Difficulty concentrating
- Confusion
- Stroke
- Pain and swelling
Deep Brain Stimulation Surgery: Frequently Asked Questions
- What is the success rate of deep brain stimulation?
In the right individuals, DBS has been observed to be a safe and effective treatment for certain conditions. While symptoms may not completely go away, many patients experience a significant improvement. Most patients will still need to take medication after undergoing DBS, but may be able to reduce their dosage — this varies from person to person.
- How long do the effects of deep brain stimulation last?
The effects of deep brain stimulation are subject to the individual’s treatment plan. Batteries can last up to 5 years in non-rechargeable impulse generators, and up to 9 years in rechargeable batteries.
- Does DBS cause personality changes?
There’s not enough empirical data available to definitively say.
- Can the effects of DBS be reversed?
Yes, the electrical stimulation is reversible. If an individual’s disease changes or his or her response to other treatments change, DBS can be adjusted.
- Does DBS damage brain tissue?
No, DBS does not cause permanent damage to any portion of the brain. However, deep brain stimulation surgery has been observed to worsen thinking and memory problems; therefore, it is not recommended for patients who have dementia.
Key Takeaways
While deep brain stimulation can be an effective treatment for essential tremor, the risks of this surgical procedure may mean it’s not always the right treatment option.
Cala Trio is a safe and less invasive alternative to DBS, and has been proven to successfully reduce the effects of hand tremor in patients living with essential tremor. If you’re interested in learning more about how to treat your essential tremor using our advanced technology, or you’re a health care professional looking for new treatment therapies for patients, contact us today.